1. Keratoconus Treatment: Solutions to Correct Your Eye Sight
Keratoconus is known as progressive eye disease, which means that your vision can continue to get worse with time. If you have been diagnosed with keratoconus, then the most important thing you can do is maintain regular appointments with your eye doctor to determine the best keratoconus treatments for your needs.
2. Keratoconus Causes
When a person is diagnosed with keratoconus, it means that the cornea becomes thin and it begins to bulge to form a cone shape. Since the cornea is shaped like a cone, it affects the way light enters the eye. Vision is distorted as a result of the light deflection that occurs away from the retina.
In most situations, a person is diagnosed with keratoconus as a teenager or in their early 20’s. Like other eye diseases, early diagnosis is best to minimize the progression of keratoconus.
Eye care researchers are still working to determine the exact cause of keratoconus. This eye disease is associated with various risk factors, including:
- Imbalance of enzymes within the cornea
- Overexposure to UV rays
- Chronic eye irritation
- History of poorly fitted contact lenses
- Excessive eye rubbing
3. Keratoconus Symptoms
During your eye exam, your optometrist will look for specific symptoms that indicate keratoconus. These signs might include:
- Progressive nearsightedness
- Blurred vision
- Light and glare sensitivity
- Changes in eyeglass prescription at every eye exam
4. Keratoconus Diagnosis: What to Expect
What should you expect when visiting an eye doctor for diagnosis? The optometrist uses several specific methods to determine if you have keratoconus of the eye:
- Keratometry: This eye test uses a circle of light that is placed on the cornea. Then, measurements are used to determine the reflection in the eye and identify the shape of the cornea.
- Corneal Mapping: Technology can be used to help with the diagnosis of a variety of eye conditions. Corneal mapping is a computerized process that records images of your cornea. These photographic tests include corneal topography and optical coherence tomography. The goal is to create a detailed map of the surface of the cornea. This information can also be used to measure corneal thickness.
- Eye Refraction: When you visit the eye doctor, it is common for the optometrist to use special equipment to determine your best vision. You will look through a device that is built with various lenses and wheels. The eye doctor changes the lenses and asks you to identify the clearest vision, helping to identify the best combination for your corrective lenses.
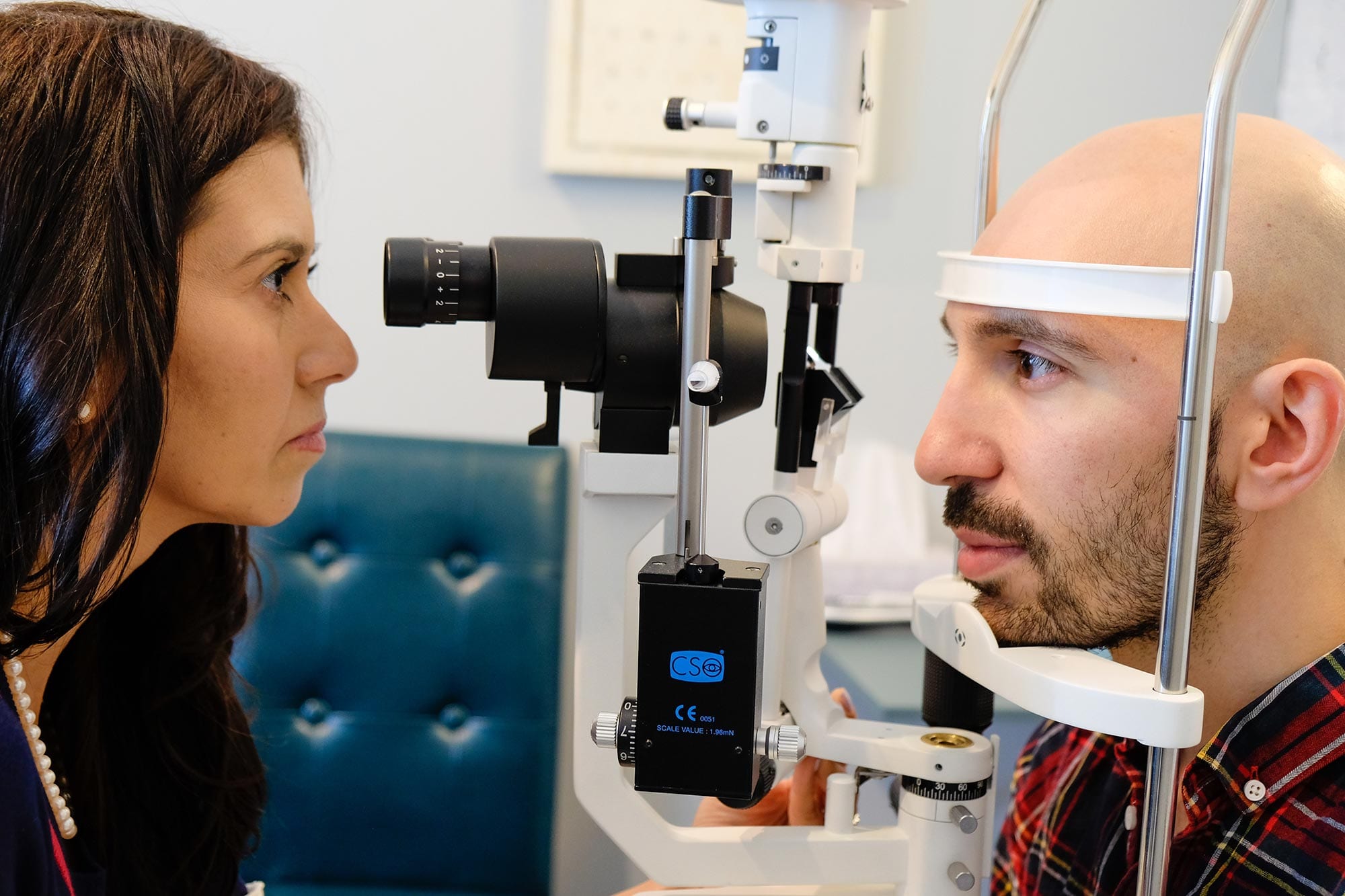
- Slit Lamp: This test involves using a vertical beam of light that is shone on your eye surface. At the same time, a low-powered microscope can be used to look at the shape of your cornea.
5. Keratoconus Treatment: Understanding Your Options
Once you have been diagnosed with keratoconus, the conversation will shift to potential treatments that can be used to correct your eyesight. Treatments vary depending on the severity of the condition and how fast it is progressing.
Patients with mild or moderate keratoconus can often use contact lenses or eyeglasses for vision correction. In many situations, vision correction lenses are beneficial to help the cornea become stable after a few years of using these lenses. If your cornea stabilizes, then you likely won’t require additional treatments in the future.
In severe cases of keratoconus, the cornea can become scarred, which makes it difficult to wear contact lenses. As a result, surgery might be recommended.
5.1 Keratoconus Contact Lenses
Contact lenses are a common choice for patients with keratoconus due to the convenience and comfort of the lenses. Keep in mind that it is common for keratoconus patients to need to change prescriptions regularly due to the changing shape of the cornea. In the early stages of keratoconus, glasses or soft contact lenses can be used.
The next step for keratoconus treatment is to use hard contact lenses (known as rigid, gas permeable lenses), or customized soft lenses. This treatment might seem uncomfortable in the beginning, but you can adjust to the feel of wearing these contact lenses. The lenses are designed to fit the shape of your cornea.
Another option is to use hybrid lenses which are designed with a rigid center and a soft outer ring to improve comfort. When patients can’t tolerate the use of hard lenses, then a hybrid is an alternative that can be tried.
When a patient has a very irregular shape of the cornea, then it means that they have reached the advanced stages of keratoconus. Scleral contact lenses might be the best treatment. Instead of having lenses that rest on the cornea (like traditional contacts), these lenses are designed to sit on the white part of your eye. The lens arches over the cornea without coming in contact with that part of your eye.
When these advanced contact lenses are required, it is essential that you work with an eye doctor who specializes in fitting keratoconus contact lenses. Additionally, regular checkups are required to ensure the proper fit of the lenses. If the contact lenses are ill-fitting, they could potentially damage the cornea and lead to additional vision issues in the future.
6. Keratoconus Stages: Determining the Right Treatment
One treatment therapy that might be recommended is known as corneal cross-linking. This procedure involves saturating the cornea with riboflavin drops. Then the cornea is treated using an ultraviolet light. Keratoconus cross-linking has been found to decrease the risk of vision loss progressing. The goal is to stabilize the cornea in the early keratoconus stages, helping to prevent further vision loss.
Sometimes, surgery might be required when keratoconus has progressed to severe stages. Surgery is recommended when a patient has corneal scarring, an inability to wear contact lenses or severe thinning of the cornea. There are two main surgical options that are commonly used:
- Corneal Inserts: Small plastic inserts can be strategically placed in the eye, helping to flatten the cone-shape of the cornea.
- Cornea Transplant: A full cornea transplant can be done when corneal scarring or thinning prevent other types of treatment.
7. Schedule an Eye Exam
Our team is here to help you maintain healthy eyes and great vision. Whether you need keratoconus treatment or you are suffering from another eye disease, we are here to help. Call today (773-360-8900) to schedule an exam and learn more.